Trapped Nerve in the Neck (Cervical Radiculopathy): Symptoms, Diagnosis & Treatment
A trapped nerve in the neck — medically known as cervical radiculopathy — is a common cause of neck and arm pain. It can lead to pain, tingling, numbness or weakness that travels from the neck down into the arm and sometimes into the hand and fingers.
This article explains :-
- What cervical radiculopathy is
- Why it happens
- How it’s diagnosed
- When you might need a scan
- Treatment options — from self-help to surgery
- What recovery typically looks like
The information can also be seen in video format below.
What Is Cervical Radiculopathy?
The term breaks down like this:
- Cervical = neck
- Radicular = relating to a spinal nerve root
- Pathy = problem or disease
So cervical radiculopathy means a problem affecting one of the nerve roots in your neck.
Understanding the Anatomy
- There are 7 vertebrae in the neck (C1–C7).
- There are 8 pairs of cervical nerve roots (C1–C8).
- These nerves exit through small openings between the vertebrae called the intervertebral foramina.
- After exiting the spine, they travel into the arm to provide:
- Sensation (feeling)
- Muscle control
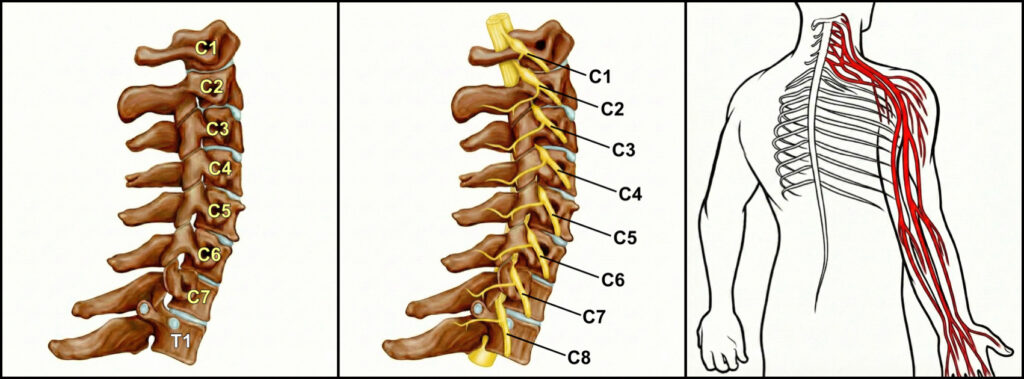
If one or more of these nerve roots becomes compressed or irritated as it leaves the spine, symptoms can develop.
What Symptoms Does It Cause?
Common symptoms include:
- Neck pain
- Pain spreading into the shoulder blade (scapular region)
- Pain travelling down the arm
- Tingling or “pins and needles”
- Numbness in the hand or fingers
- Occasionally, weakness in the arm or hand
Arm Pain Radiation
Each nerve root supplies a certain area of the arm with sensation. The area supplied by a nerve root is called its ‘dermatome’. The most common nerves affected by cervical radiculogpthy are the C6, 7 and C8 nerve roots, which are the ones whose dermatomes supply the hand. Hand and finger pain / tingling is a common symptom when these nerve root are irritated.
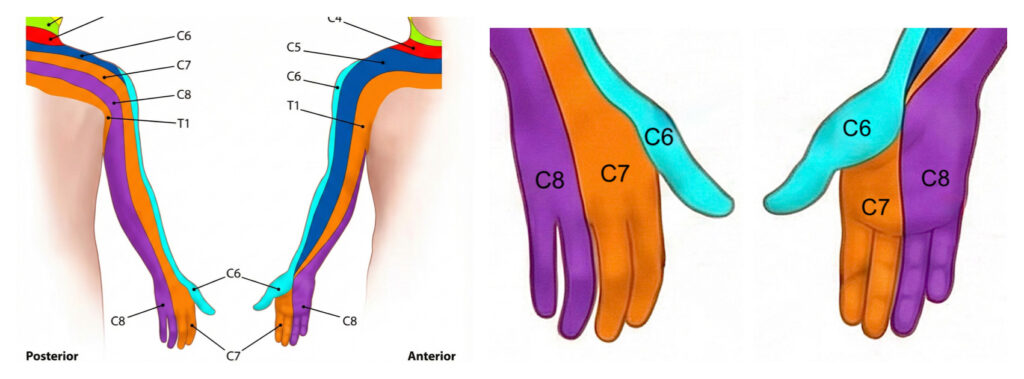
- C6 – Often radiates into the thumb
- C7 – Often affects the middle finger
- C8 – Often affects the little finger
However, there is considerable overlap between individuals. Symptoms do not always follow textbook patterns.
A Note About Weakness
Muscle weakness is less common but more significant. It may suggest more substantial nerve compression and should be assessed promptly. This may present as shoulder, elbow or wrist weakness, grip weakness or a lack of hand and finger dexterity.
Red Flag Symptoms – When to Seek Urgent Help
Although most cases are not dangerous, seek urgent medical assessment (A&E or urgent care) if you develop:
- Progressive weakness in one or both arms
- Sudden leg weakness
- Problems with walking or balance
- New bladder or bowel control issues
These symptoms may indicate spinal cord compression and require urgent investigation.
Why Does Cervical Radiculopathy Happen?
The nerve roots are vulnerable where they exit the spine through the intervertebral foramen. Anything that narrows this space can irritate or compress the nerve.
Common Causes
In younger people:
- Disc bulge or disc prolapse
In older adults:
- Osteoarthritis
- Bony outgrowths called osteophytes
Sometimes both occur together — this is known as a disc–osteophyte complex.
Does Severity on a Scan Match Symptoms?
Not always.
- Mild compression can sometimes cause severe pain.
- Severe compression can occasionally cause less pain but more weakness or constant numbness.
Symptoms don’t always match imaging findings perfectly.
How Is It Diagnosed?
Cervical radiculopathy is usually diagnosed clinically.
This means a healthcare professional will:
- Listen to your symptoms
- Examine neck movement
- Test strength, sensation and nerve function in your arms
Do You Need an MRI Scan?
In most early cases — no.
An MRI scan may be recommended if:
- Symptoms are severe
- There is significant or progressive weakness
- Symptoms are not improving after 6–12 weeks
- Red flag symptoms are present
In many cases during the first few weeks, a scan simply confirms what is already suspected and does not change management.
Treatment for a Trapped Nerve in the Neck
The good news is that most cases improve over time.
How Long Does It Take to Recover?
- Most improve within 6–12 weeks
- Some can take up to 3 months
- The vast majority settle without surgery
Nerves can adapt and inflammation can reduce naturally over time.
Pain Relief
Because pain can be significant and disrupt sleep, medication is often used to keep symptoms manageable while recovery occurs.
Common options include:
- Paracetamol (acetaminophen)
- Anti-inflammatory medication
- Codeine-based medication (short term)
- Neuropathic pain medication (in some cases)
Always follow medical advice when taking medication.
Sleep Advice
Sleep can be one of the most difficult aspects of this condition.
Certain neck positions narrow the space around the nerve root:
- Side bending toward the painful side can increase pressure
- Neck extension (looking upwards) can narrow the foramina on both sides

Positions That Often Help
- Lying on your back
- Lying on your non-painful side
- Supporting the painful arm on a pillow
There is no single “perfect” position. The best position is the one that feels most comfortable for you.
Taking pain medication about an hour before bed may also help improve sleep quality.
Exercises and Movement
Gentle movement is helpful. Avoid :-
- Prolonged bed rest
- Holding the neck in one position for long periods
- Sustained neck flexion (looking down)
- Sustained neck extension (looking up)
Helpful approaches include:
- Gentle neck rotation movements
- Shoulder pendular exercises
- Frequent short movement breaks during the day
Let pain guide you. Avoid aggressive stretching or forceful exercises that worsen symptoms.
Do You Need a Scan Early?
In most cases, early scanning is not required.
However, an MRI may be considered sooner if:
- Red flag symptoms are present
- Weakness is progressive
- Pain is severe and intolerable
Otherwise, conservative management is usually recommended first.
What If It Doesn’t Improve After 3 Months?
If symptoms have not improved after around 3 months, an MRI scan is usually appropriate.
At that stage:
- Recovery is less likely to occur spontaneously
- Injections or surgery may be considered
- Surgeons will require recent imaging to plan treatment
Getting a scan too early often means it will need repeating later.
Injection or Surgery
If symptoms persist and imaging confirms nerve compression, options may include:
1. Nerve Root Injection
- A steroid injection around the affected nerve
- Aims to reduce inflammation and pain
- May allow symptoms to settle without surgery
2. Surgery
If compression is significant or symptoms are severe, surgery may be recommended.
The most common procedure is:
Anterior Cervical Decompression and Fusion (ACDF)
This involves:
- A small incision at the front of the neck
- Removal of the disc or bone pressing on the nerve
- Fusing the adjacent vertebrae using metalwork
It is a routine procedure performed under general anaesthetic, but as with all surgery, there are risks. A spinal surgeon would discuss individual risks and benefits with you.
Summary
If you have a trapped nerve in your neck:
- Try not to panic
- Most cases improve within a few months
- Early scans are not usually necessary
- Gentle movement and pain control are key
- Seek urgent help if red flag symptoms develop
If symptoms are severe or not improving, speak to a healthcare professional for further assessment and guidance.
